Anterior Cervical Discectomy with Fusion, One Level (Includes Implants & Hardware)
Anterior Cervical Discectomy with Fusion, One Level
A level may be performed when a herniated disc pinches a nerve in the neck, and non-surgical treatment has not resulted in sufficient relief. The primary symptoms of an Anterior Cervical Discectomy are usually numbness, weakness, and/or pain in the arm and neck. The goal of the Anterior Cervical Discectomy with Fusion is to remove the disc that is pinching the nerve, eliminating the cause of pain and numbness. One level Anterior Cervical Discectomy with Fusion involves One Disc.
FAQS
Frequently asked questions about surgical procedures
Can I use my insurance and get these prices?
Payment is due 14 calendar days prior to your surgery date. If, after the cutoff, your account is not settled, your case must be postponed.
How quickly can I have surgery?
How will I meet my surgeon?
If I had a car or work accident, would you work with my employer or attorney for payment?
What if I get sick right before my surgery?
You could develop a respiratory infection, a urinary tract infection, COVID, or some other condition that may necessitate postponement. There is no penalty when this happens.
Preparation before surgery
You may be scheduled for presurgical tests (blood test, electrocardiogram, chest X-ray) several days before surgery. In the doctor’s office, you will sign consent and other forms so that the surgeon knows your medical history (allergies, medicines, vitamins, bleeding history, anesthesia reactions, and previous surgeries). Discuss all medications (prescription, over-the-counter, and herbal supplements) you are taking with your health care provider. Some medications need to be continued or stopped the day of surgery. Stop taking all non-steroidal anti-inflammatory medicines (Naprosyn, Advil, Motrin, Nuprin, Aleve, etc.) and blood thinners (Coumadin, Plavix, etc.) 1 to 2 weeks before surgery as directed by the doctor. Additionally, stop smoking, chewing tobacco, and drinking alcohol 1 week before and 2 weeks after surgery because these activities can cause bleeding problems. No food or drink is permitted past midnight the night before surgery.
What’s Included:
- Facility fee
- Graft and hardware costs (if needed)
- Surgeon and assistant surgeon fees
- Anesthesiologist
- Time in the recovery unit (at no additional charge)
- Initial consultation visit
- One post-operative visit
*Please note: If you choose not to proceed with surgery after the initial consultation, or if you delay your procedure for more than 6 weeks, you will need to update your consultation at a cost of $375.
What’s not included:
- Lab testing before and after the surgery, as needed
- Electrocardiogram (EKG), depending on age. If you had one elsewhere in the past 6 months and it read “normal”, we can forego this expense.
- Imaging costs. X-rays and MRIs can be obtained anywhere.
- Physical therapy services
- Medications you’ll need (oral or IV antibiotic infusions if an infection arises)
- Wound care
- Bracing supplies
- Additional doctor visits (a pre-operative visit with the surgeon, in person, and any required post-op follow-ups after the suture removal to monitor your progress
- Additional surgical intervention if a complication arises
- Additional imaging or hospital care if a blood clot develops
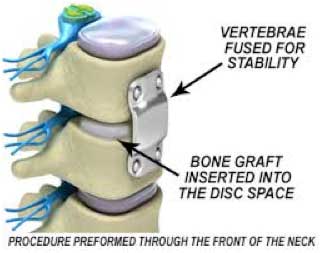
Anterior Cervical Discectomy with Fusion, One Level Surgery
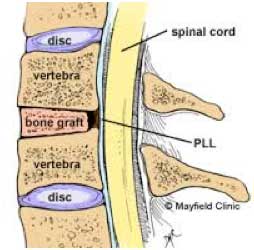
The incision is made in the front of the spine through the throat area. After the disc is removed, a bone graft is inserted to fuse together the bones above and below the disc space. Discectomy literally means “cutting out the disc.” A discectomy can be performed anywhere along the spine from the neck (cervical) to the low back (lumbar). The surgeon reaches the damaged disc from the front (anterior) of the spine through the throat area. By moving aside the neck muscles, trachea, and esophagus, the disc and bony vertebrae are exposed. Surgery from the front of the neck is more accessible than from the back (posterior) because the disc can be reached without disturbing the spinal cord, spinal nerves, and the strong neck muscles. Depending on your particular symptoms, one disc (single-level) or more (multi-level) may be removed. After the disc is removed, the space between the bony vertebrae is empty. To prevent the vertebrae from collapsing and rubbing together, a spacer bone graft is inserted to fill the open disc space. The graft serves as a bridge between the two vertebrae to create a spinal fusion. The bone graft and vertebrae are fixed in place with metal plates and screws.
Recovery
Following surgery, the body begins its natural healing proces, and new bone cells grow around the graft. After 3 to 6 months, the bone graft should join the two vertebrae and form one solid piece of bone. The instrumentation and fusion work together, similar to reinforced concrete. You must wear your collar at all times except to shower, and you may remove it briefly for personal hygiene (shaving). While the collar is off, you may look forward or slightly downward, but you must not look up. This motion extends your neck and can cause the bone graft to dislodge. Most people will need to wear the collar until the first post-operative appointment. At that time, I will determine if you are able to stop using the collar. In most cases, a collar will be worn for about 3-4 weeks. Some patients may have to continue to wear the collar for a longer period of time, depending on their situation
Risks
Anterior Cervical Discectomy and Fusion (ACDF) is generally a safe and effective surgery. However, as with any surgical procedure, there are potential risks. Risks of the operation include, but are not limited to: infection, anesthesia complications, injury to the nerves and spinal cord, hoarseness, injury to the esophagus, incomplete resolution of pain, and dislodgement of the graft. General medical complications include pneumonia, heart attack, stroke, and blood clots. These complications are uncommon, and many precautions are taken to prevent or minimize risk,s but because human biology is at times unpredictable, no surgery is risk-free.
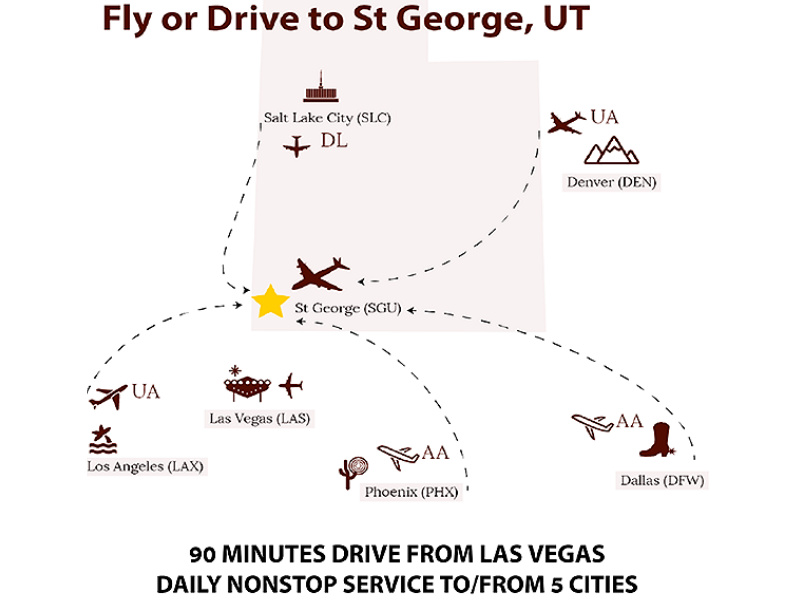
Can I Travel to St George for Surgery?
Yes, and we’ll help you make all your arrangements.
- We have arrangements to try to obtain free flights through a non-profit volunteer pilot organization. We can do this with 10 days’ advance notice in most cases.
- We have discount codes for the Holiday Inn in town. This hotel is 1.5 miles from the surgery center and 2 miles from our clinic.
- We’ll arrange to send your after-surgery medications to your hometown pharmacy for pickup before you leave.
What if I would rather drive to St George?
No problem, we can help with those plans as well. When you have surgery with us, we’ll need to make sure you’re safe and comfortable after surgery. We’ll arrange cold compression therapy that requires an AC/DC adaptor/transformer and frequent stops to stretch and refill the ice reservoir on the road.
We’ll ask about the vehicle you’ll travel in to ensure you have a way to elevate and stretch out in the vehicle on the road while someone else does the driving.
How are follow-up and initial consultations handled?
In-person and telehealth consultations are possible with the surgeon to whom your case is assigned. The initial visit is included in the surgical package and is valued at $375.
We can also obtain the flights from the volunteer pilot nonprofit if you’d like to come for initial and follow-up visits in person. One follow-up visit is included in the surgical package at a value of $175. Any additional visits are charged at the time of service to your credit or debit card.
Transparent Pricing Guide
Find out the exact cost of your procedure in seconds, with no hidden fees, no surprises, and complete transparency every step of the way.
